How do Diabetic Foot Ulcers Form?
A diabetic foot ulcer is an open wound or sore, which can be a red, shallow crater on the foot. Foot ulcers are usually superficial, involving only the surface of the skin; however, among diabetics, foot ulcers can get deep into the skin and tissue involving deep structures including tendons and bones.
How do Diabetic Foot ulcers form?
Some patients who have diabetes for many years can develop neuropathy. This is a condition where the patient has decreased sensation or worse, can no longer feel their foot due to nerve damage cause by chronic elevated blood sugars. This lack of sensation can lead to foot deformities.
Also, patients with diabetes are prone to vascular disease, which further complicates the healing of foot ulcers. Due to poor blood circulation around the foot, there is a delay for healing factors and other blood components like white blood cells (which defend the body from infections) to reach the affected area. This is the reason why some diabetic patients have wounds that heal very slowly.
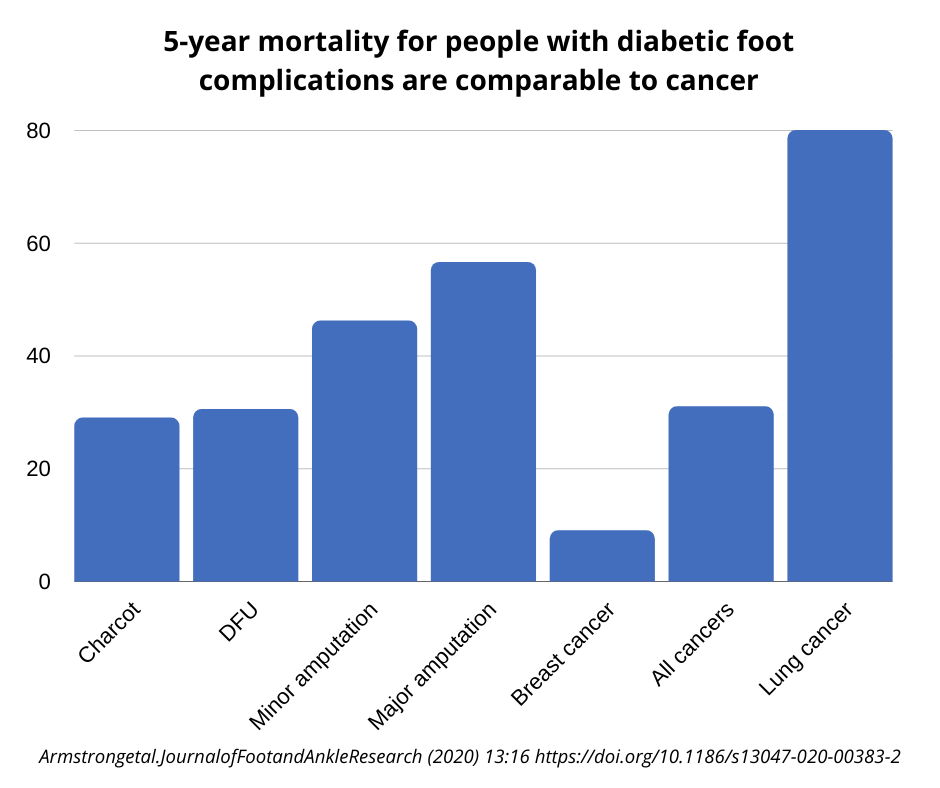
Why you should take a foot ulcer seriously?
This is very important especially among diabetics. Once you notice a foot wound or ulcer that does not heal or heals very slowly, schedule an appointment with your podiatrist immediately to:
· Reduce the risk of infection.
· Reduce the risk of an amputation.
· Improve functionality of your feet.
· Improve quality of life.
How to Prevent a Foot Ulcer
Prevention is always better than treatment. The best way to do this is to seek consult from your podiatrist. You doctor will determine if you are at high risk for developing foot ulcer and will provide a plan for you.
Typically, you are high risk if you
· Have high or uncontrolled blood sugar levels.
· Have signs of foot deformity such as a bunion or hammer toe.
· Have decreased foot sensation
· Have poor blood circulation
Common recommended ways to prevent foot ulcers include:
· Control and maintain blood sugar levels.
· Use proper foot wear.
· Check feet daily. Look out for cuts, wounds, fungal growth, foot odor, corns, calluses and if you notice any of these, have it seen by your podiatrist.
· Exercise daily
· Follow a good diet plan
It is recommended to regularly see a podiatrist once or twice a year; whether or not you think you have a foot problem. A comprehensive foot examination will determine the risk factors that may result in foot ulcers or worse, consequent foot amputation.
If you develop a foot wound, have it checked immediately. Call your podiatrist to schedule an appointment as soon as possible.
For more information on diabetic foot ulcers, you may contact Advanced Wound Healing Institute at (239) 430-3668 (FOOT). Advanced Wound Healing Institute is part of Family Foot and Leg Center, P.A.
- Faster recovery time
- Better results
- Improved long-term outlook
- Optimal quality of life
Self Service Portal open
24 hrs/7 days
Our doctors are well trained from residency in conservative and advanced wound care options from simple debridement to advance grafting and flap techniques.
At the Advanced Wound Healing Institute, we specialize in the treatment of wounds that are difficult to heal. We offer the most current and advanced treatments in wound care.
If you or your loved ones suffer from diabetes, must see us now. What you need to know now.